Animal Testing
peta.org
Animal testing, also known as animal experimentation, animal research and in vivo testing, is the use of non-human animals in experiments that seek to control the variables that affect the behavior or biological system under study.
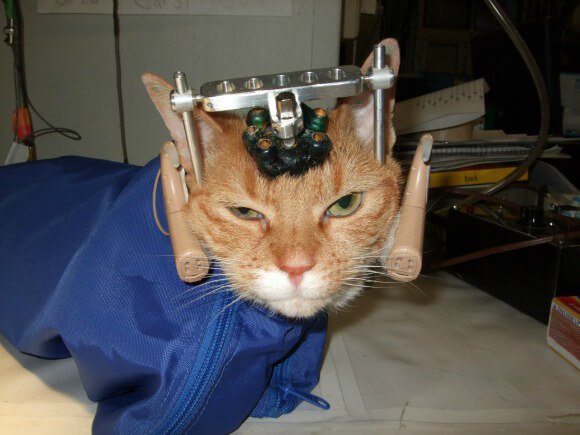
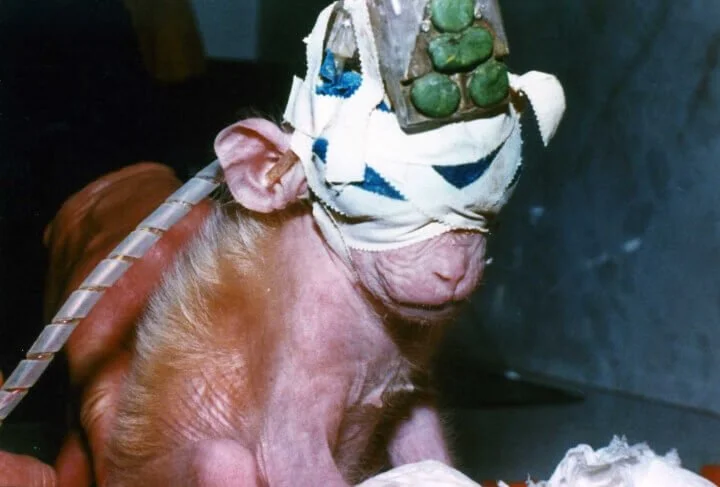
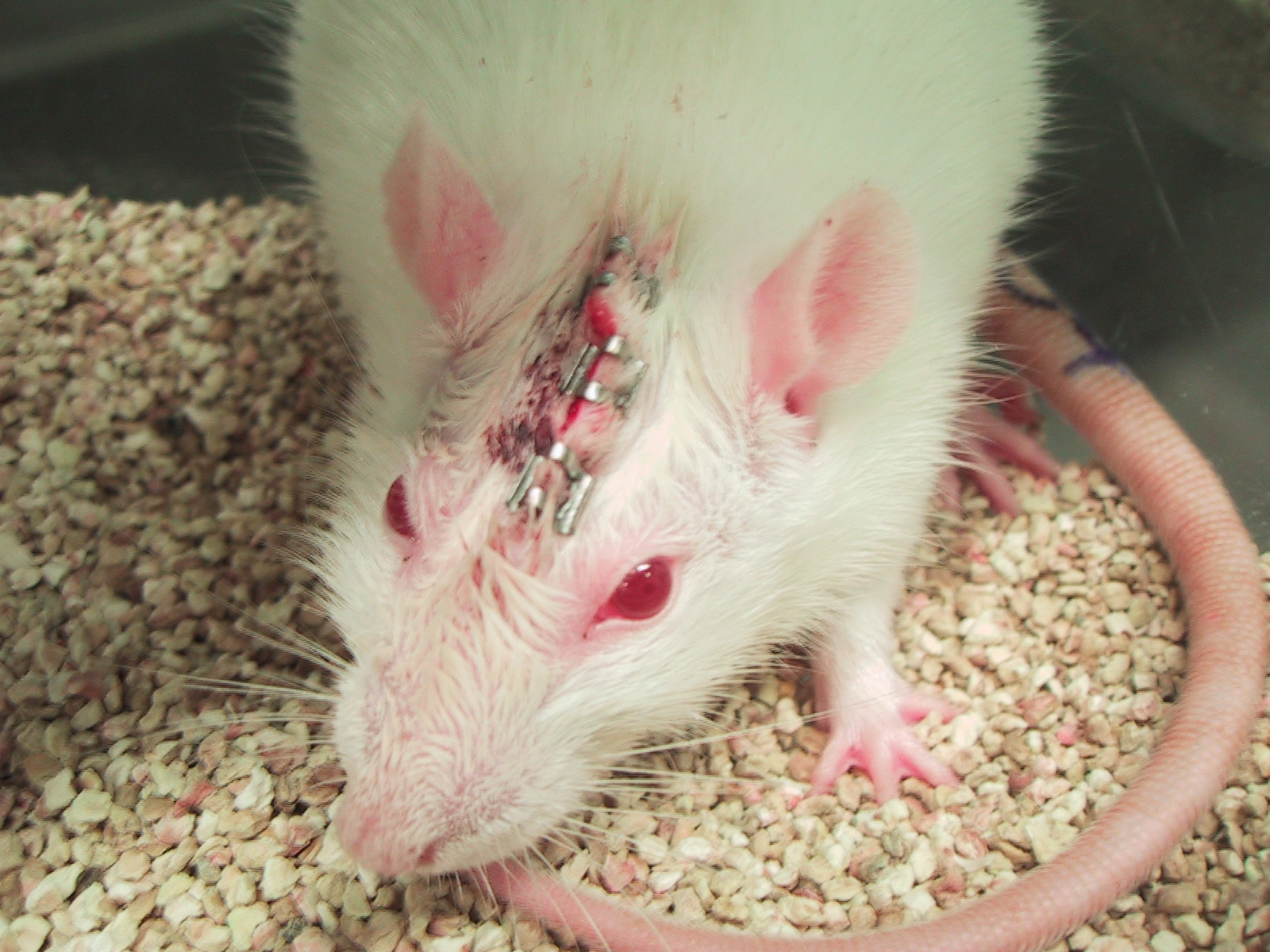
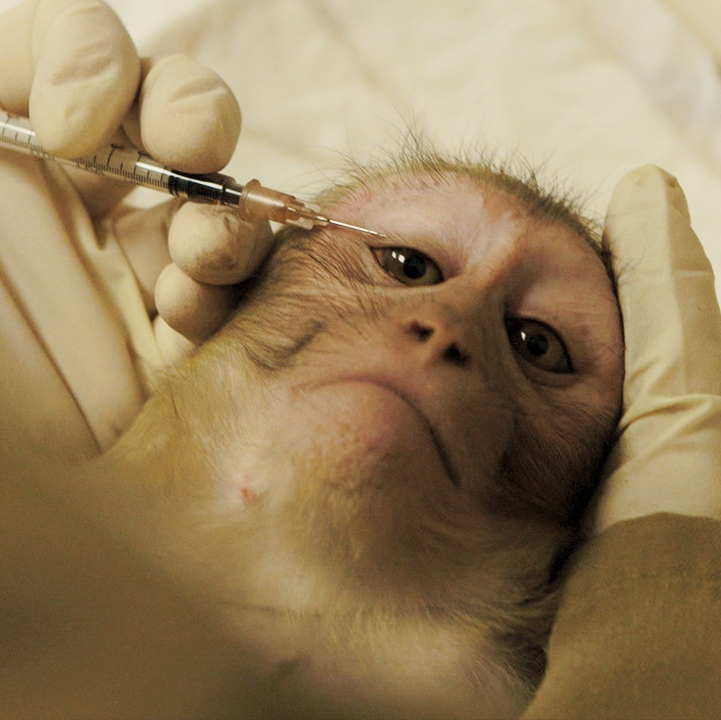
Each year, more than 100 million animals—including mice, rats, frogs, dogs, cats, rabbits, hamsters, guinea pigs, monkeys, fish, and birds—are killed in U.S. laboratories for biology lessons, medical training, curiosity-driven experimentation, and chemical, drug, food, and cosmetics testing. Before their deaths, some are forced to inhale toxic fumes, others are immobilized in restraint devices for hours, some have holes drilled into their skulls, and others have their skin burned off or their spinal cords crushed. In addition to the torment of the actual experiments, animals in laboratories are deprived of everything that is natural and important to them—they are confined to barren cages, socially isolated, and psychologically traumatized. The thinking, feeling animals who are used in experiments are treated like nothing more than disposable laboratory equipment.
Wasteful and Unreliable
Pew Research Center poll have found that 50 percent of U.S. adults oppose the use of animals in scientific research, and other surveys suggest that the shrinking group that does accept animal experimentation does so only because it believes it to be necessary for medical progress.(1,2) The reality is that the majority of animal experiments do not contribute to improving human health, and the value of the role that animal experimentation plays in most medical advances is questionable.
In an article published in The Journal of the American Medical Association, researchers found that medical treatments developed in animals rarely translated to humans and warned that “patients and physicians should remain cautious about extrapolating the finding of prominent animal research to the care of human disease … poor replication of even high-quality animal studies should be expected by those who conduct clinical research.”(3)
Diseases that are artificially induced in animals in a laboratory, whether they be mice or monkeys, are never identical to those that occur naturally in human beings. And because animal species differ from one another biologically in many significant ways, it becomes even more unlikely that animal experiments will yield results that will be correctly interpreted and applied to the human condition in a meaningful way.
For example, according to former National Cancer Institute Director Dr. Richard Klausner, “We have cured mice of cancer for decades, and it simply didn’t work in humans.”(4) This conclusion was echoed by former National Institutes of Health (NIH) Director Dr. Elias Zerhouni, who acknowledged that experimenting on animals has been a boondoggle. “We have moved away from studying human disease in humans,” he said. “We all drank the Kool-Aid on that one, me included. … The problem is that it hasn’t worked, and it’s time we stopped dancing around the problem. … We need to refocus and adapt new methodologies for use in humans to understand disease biology in humans.”(5)
Britches
The data is sobering: Although at least 85 HIV/AIDS vaccines have been successful in nonhuman primate studies, as of 2015, every one has failed to protect humans.(6) In one case, an AIDS vaccine that was shown to be effective in monkeys failed in human clinical trials because it did not prevent people from developing AIDS, and some believe that it made them more susceptible to the disease. According to a report in the British newspaper The Independent, one conclusion from the failed study was that “testing HIV vaccines on monkeys before they are used on humans, does not in fact work.”(7)
These are not anomalies. The U.S. Food and Drug Administration has stated, “Currently, nine out of ten experimental drugs fail in clinical studies because we cannot accurately predict how they will behave in people based on laboratory and animal studies.”(8)
Research published in the journal Annals of Internal Medicine revealed that universities commonly exaggerate findings from animal experiments conducted in their laboratories and “often promote research that has uncertain relevance to human health and do not provide key facts or acknowledge important limitations.”(9) One study of media coverage of scientific meetings concluded that news stories often omit crucial information and that “the public may be misled about the validity and relevance of the science presented.”(10) Because experimenters rarely publish results of failed animal studies, other scientists and the public do not have ready access to information on the ineffectiveness of animal experimentation.
occupyforanimals.net
Funding and Accountability
Through their taxes, charitable donations, and purchases of lottery tickets and consumer products, members of the public are ultimately the ones who—knowingly or unknowingly—fund animal experimentation. One of the largest sources of funding comes from publicly funded government granting agencies such as NIH. Approximately 47 percent of NIH-funded research involves experimentation on nonhuman animals, and in 2012, NIH budgeted nearly $30 billion for research and development.(11,12) In addition, many charities––including the March of Dimes, the American Cancer Society, and countless others—use donations to fund experiments on animals. One-third of the projects funded by the National Multiple Sclerosis Society involve animal experimentation.(13) Visit HumaneSeal.org to find out which charities do and which do not fund research on animals.
Despite the vast amount of public funds being used to underwrite animal experimentation, it is nearly impossible for the public to obtain current and complete information regarding the animal experiments that are being carried out in their communities or funded with their tax dollars. State open-records laws and the U.S. Freedom of Information Act can be used to obtain documents and information from state institutions, government agencies, and other federally funded facilities, but private companies, contract labs, and animal breeders are exempt. In many cases, institutions that are subject to open-records laws fight vigorously to withhold information about animal experimentation from the public.(14)
Oversight and Regulation
Despite the countless animals killed each year in laboratories worldwide, most countries have grossly inadequate regulatory measures in place to protect animals from suffering and distress or to prevent them from being used when a non-animal approach is readily available. In the U.S., the species most commonly used in experiments (mice, rats, birds, fish, reptiles, and amphibians) comprise 99% of all animals in laboratories but are specifically exempted from even the minimal protections of the federal Animal Welfare Act (AWA).(15,16) Many laboratories that use only these species are not required by law to provide animals with pain relief or veterinary care, to search for and consider alternatives to animal use, to have an institutional committee review proposed experiments, or to be inspected by the U.S. Department of Agriculture (USDA) or any other entity. Some estimates indicate that as many as 800 U.S. laboratories are not subject to federal laws and inspections because they experiment exclusively on mice, rats, and other animals whose use is largely unregulated.(17)
As for the more than 11,000 facilities that the USDA does regulate (of which more than 1,200 are designated for “research”), only 120 USDA inspectors are employed to oversee their operations.(18) Reports have repeatedly concluded that even the minimal standards set forth by the AWA are not being met by these facilities, and institutionally based oversight bodies, called Institutional Animal Care and Use Committees (IACUCs), have failed to carry out their mandate. A 1995 report by the USDA’s Office of the Inspector General (OIG) “found that the activities of the IACUCs did not always meet the standards of the AWA. Some IACUCs did not ensure that unnecessary or repetitive experiments would not be performed on laboratory animals.”(19) In 2000, a USDA survey of the agency’s laboratory inspectors revealed serious problems in numerous areas, including “the search for alternatives [and] review of painful procedures.”(20) A September 2005 audit report issued by the OIG found ongoing “problems with the search for alternative research, veterinary care, review of painful procedures, and the researchers’ use of animals.”(21) In December 2014, an OIG report documented continuing problems with laboratories failing to comply with the minimal AWA standards and the USDA’s weak enforcement actions failing to deter future violations. The audit highlighted that from 2009 to 2011, USDA inspectors cited 531 experimentation facilities for 1,379 violations stemming from the IACUCs’ failure to adequately review and monitor the use of animals. The audit also determined that in 2012, the USDA reduced its penalties to AWA violators by an average of 86 percent, even in cases involving animal deaths and egregious violations.(22)
Research co-authored by PETA documented that, on average, animal experimenters and laboratory veterinarians comprise a combined 82 percent of the membership of IACUCs at leading U.S. institutions. A whopping 98.6 percent of the leadership of these IACUCs was also made up of animal experimenters. The authors observed that the dominant role played by animal experimenters on these committees “may dilute input from the few IACUC members representing animal welfare and the general public, contribute to previously-documented committee bias in favor of approving animal experiments and reduce the overall objectivity and effectiveness of the oversight system.”(23) Even when facilities are fully compliant with the law, animals who are covered can be burned, shocked, poisoned, isolated, starved, forcibly restrained, addicted to drugs, and brain-damaged. No procedures or experiments, regardless of how trivial or painful they may be, are prohibited by federal law. When valid non-animal research methods are available, no federal law requires experimenters to use such methods instead of animals.
The Way Forward
A high-profile study published in the prestigious BMJ (formerly British Medical Journal) documenting the ineffectiveness and waste of experimentation on animals concluded that “if research conducted on animals continues to be unable to reasonably predict what can be expected in humans, the public’s continuing endorsement and funding of preclinical animal research seems misplaced.”(24)
Research with human volunteers, sophisticated computational methods, and in vitro studies based on human cells and tissues are critical to the advancement of medicine. Cutting-edge non-animal research methods are available and have been shown time and again to be more accurate than crude animal experiments.(25) However, this modern research requires a different outlook, one that is creative and compassionate and embraces the underlying philosophy of ethical science. Human health and well-being can also be promoted by adopting nonviolent methods of scientific investigation and concentrating on the prevention of disease before it occurs, through lifestyle modification and the prevention of further environmental pollution and degradation. The public is becoming more aware and more vocal about the cruelty and inadequacy of the current research system and is demanding that tax dollars and charitable donations not be used to fund experiments on animals.
References
1) Cary Funk and Lee Rainie, “Public and Scientists’ Views on Science and Society,” Pew Research Center, 29 Jan. 2015.
2) Peter Aldhous and Andy Coghlan, “Let the People Speak,” New Scientist 22 May 1999.
3) Daniel G. Hackam, M.D., and Donald A. Redelmeier, M.D., “Translation of Research Evidence From Animals to Human,” The Journal of the American Medical Association 296 (2006): 1731-2.
4) Marlene Simmons et al., “Cancer-Cure Story Raises New Questions,” Los Angeles Times 6 May 1998.
5) Rich McManus, “Ex-Director Zerhouni Surveys Value of NIH Research,” NIH Record 21 June 2013.
6) Jarrod Bailey, “An Assessment of the Role of Chimpanzees in AIDS Vaccine Research,” Alternatives to Laboratory Animals 36 (2008): 381-428.
7) Steve Connor and Chris Green, “Is It Time to Give Up the Search for an AIDS Vaccine?” The Independent 24 Apr. 2008.
8) U.S. Food and Drug Administration, “FDA Issues Advice to Make Earliest Stages of Clinical Drug Development More Efficient,” FDA News Release 12 Jan. 2006.
9) Steve Woloshin, M.D., M.S., et al., “Press Releases by Academic Medical Centers: Not So Academic?” Annals of Internal Medicine 150 (2009): 613-8.
10) Steven Woloshin and Lisa Schwartz, “Media Reporting on Research Presented at Scientific Meetings: More Caution Needed,” The Medical Journal of Australia 184 (2006): 576-80.
11) Diana E. Pankevich et al., “International Animal Research Regulations: Impact on Neuroscience Research,” The National Academies (2012).
12) National Institutes of Health, “NIH Budget,” About NIH, 18 Nov. 2012.
13) Pankevich et al.
14) Deborah Ziff, “On Campus: PETA Sues UW Over Access to Research Records,” Wisconsin State Journal 5 Apr. 2010.
15) U.S. Department of Agriculture, Animal and Plant Health Inspection Service, “Animal Welfare, Definition of Animal,” Federal Register, 69 (2004): 31513-4.
16) Justin Goodman et al., “Trends in Animal Use at US Research Facilities,” Journal of Medical Ethics 0(2015): 1-3.
17) The Associated Press, “Animal Welfare Act May Not Protect All Critters,” 7 May 2002.
18) U.S. Department of Agriculture, Animal and Plant Health Inspection Service, “Animal Care: Search.”
19) U.S. Department of Agriculture, Office of Inspector General, “APHIS Animal Care Program, Inspection and Enforcement Activities,” audit report, 30 Sept. 2005.
20) U.S. Department of Agriculture, Animal and Plant Health Inspection Service, “USDA Employee Survey on the Effectiveness of IACUC Regulations,” Apr. 2000.
21) U.S. Department of Agriculture, Office of Inspector General, “APHIS Animal Care Program, Inspection and Enforcement Activities,” audit report, 30 Sept. 2005.
22) U.S. Department of Agriculture, Office of Inspector General, “Animal and Plant Health Inspection Service Oversight of Research Facilities,” audit report, Dec. 2014.
23) Lawrence A. Hansen et al., “Analysis of Animal Research Ethics Committee Membership at American Institutions,” Animals 2 (2012): 68-75.
24) Pandora Pound and Michael Bracken, “Is Animal Research Sufficiently Evidence Based To Be A Cornerstone of Biomedical Research?,” BMJ (2014): 348.
25) Junhee Seok et al., “Genomic Responses in Mouse Models Poorly Mimic Human Inflammatory Diseases,” Proceedings of the National Academy of Sciences 110 (2013): 3507-12.
A few facts:
Brian Gunn/IAAPEA
- Over 100 million animals are burned, crippled, poisoned, and abused in US labs every year.
- 92% of experimental drugs that are safe and effective in animals fail in human clinical trials because they are too dangerous or don’t work.
- Labs that use mice, rats, birds, reptiles and amphibians are exempted from the minimal protections under the Animal Welfare Act (AWA).
- Up to 90% of animals used in U.S. labs are not counted in the official statistics of animals tested.
- Europe, the world’s largest cosmetic market, Israel and India have already banned animal testing for cosmetics, and the sale or import of newly animal-tested beauty products.
- Even animals that are protected under the AWA can be abused and tortured. And the law doesn’t require the use of valid alternatives to animals, even if they are available.
- According to the Humane Society, registration of a single pesticide requires more than 50 experiments and the use of as many as 12,000 animals.
- In tests of potential carcinogens, subjects are given a substance every day for 2 years. Others tests involve killing pregnant animals and testing their fetuses.
- The real-life applications for some of the tested substances are as trivial as an “improved” laundry detergent, new eye shadow, or copycat drugs to replace a profitable pharmaceutical whose patent expired.
- Alternative tests achieve one or more of the “3 R’s:” replaces a procedure that uses animals with a procedure that doesn’t, reduces the number of animals used in a procedure, refines a procedure to alleviate or minimize potential animal pain.
- Several cosmetic tests commonly performed on mice, rats, rabbits, and guinea pigs include: skin and eye irritation tests where chemicals are rubbed on shaved skin or dripped into the eyes without any pain relief.
The information above is from the website www.dosomething.org
Animal Testing Q&A
“If we didn’t use animals, we’d have to test new drugs on people.”
The fact is that we already do test new drugs on people. No matter how many tests on animals are undertaken, someone will always be the first human to be tested on. Because animal tests are so unreliable, they make those human trials all the more risky. The National Institutes of Health (NIH) has noted that 95 percent of all drugs that are shown to be safe and effective in animal tests fail in human trials because they don’t work or are dangerous. And of the small percentage of drugs approved for human use, half end up being relabeled because of side effects that were not identified in tests on animals.
Vioxx, Phenactin, E-Ferol, Oraflex, Zomax, Suprol, Selacryn, and many other drugs have had to be pulled from the market in recent years because of adverse reactions experienced by people taking them. Despite rigorous animal tests, prescription drugs kill 100,000 people each year, making them our nation’s fourth-largest killer.
Fortunately, a wealth of cutting-edge non-animal research methods promises a brighter future for both animal and human health.
“We have to observe the complex interactions of cells, tissues, and organs in living animals.”
Taking healthy beings from a completely different species, artificially inducing a condition that they would never normally contract, keeping them in an unnatural and stressful environment, and trying to apply the results to naturally occurring diseases in human beings is dubious at best. Physiological reactions to drugs vary enormously from species to species (and even within a species). Penicillin kills guinea pigs but is inactive in rabbits. Aspirin kills cats and causes birth defects in rats, mice, guinea pigs, dogs, and monkeys. And morphine, a depressant in humans, stimulates goats, cats, and horses. Further, animals in laboratories typically display behavior indicating extreme psychological distress, and experimenters acknowledge that the use of these stressed-out animals jeopardizes the validity of the data produced.
Brian Gunn/IAAPEA
Sir Alexander Fleming, who discovered penicillin, remarked, “How fortunate we didn’t have these animal tests in the 1940s, for penicillin would probably have never been granted a license, and probably the whole field of antibiotics might never have been realized.” Modern non-animal research methods are faster, cheaper, and more relevant to humans than tests on animals.
Sophisticated human cell- and tissue-based research methods allow researchers to test the safety and effectiveness of new drugs, vaccines, and chemical compounds. The HμREL biochip uses living human cells to detect the effects of a drug or chemical on multiple interacting organs, VaxDesign’s Modular Immune in vitro Construct (MIMIC®) system uses human cells to create a working dime-sized human immune system for testing vaccines, and Harvard researchers have developed a human tissue-based “lung-on-a-chip” that can “breathe” and be used to estimate the effects of inhaled chemicals on the human respiratory system. Human tissue-based methods are also used to test the potential toxicity of chemicals and for research into burns, allergies, asthma, and cancer.
Clinical research on humans also gives great insights into the effects of drugs and how the human body works. A research method called microdosing can provide information on the safety of an experimental drug and how it’s metabolized in the body by administering an extremely small one-time dose that’s well below the threshold necessary for any potential pharmacologic effect to take place. Researchers can study the working human brain using advanced imaging techniques and can even take measurements down to a single neuron.
“Animals help in the fight against cancer.”
Through taxes, donations, and private funding, Americans have spent hundreds of billions of dollars on cancer research since 1971. However, the return on that investment has been dismal. A survey of 4,451 experimental cancer drugs developed between 2003 and 2011 found that more than 93 percent failed after entering the first phase of human clinical trials, even though all had been tested successfully on animals. The authors of this study point out that animal “models” of human cancer created through techniques such as grafting human tumors onto mice can be poor predictors of how a drug will work in humans.
Richard Klausner, former head of the National Cancer Institute (NCI), has observed, “The history of cancer research has been a history of curing cancer in the mouse. We have cured mice of cancer for decades and it simply didn’t work in humans.” Studies have found that the chemicals that cause cancer in rats only caused cancer in mice 46 percent of the time. If extrapolating from rats to mice is so problematic, how can we extrapolate results from mice, rats, guinea pigs, rabbits, cats, dogs, monkeys, and other animals to humans?
The NCI now uses human cancer cells, taken by biopsy during surgery, to perform first-stage testing for new anti-cancer drugs, sparing the 1 million mice the agency previously used annually and giving us all a much better shot at combating cancer.
Furthermore, according to the World Health Organization, cancer is largely preventable, yet most health organizations that focus on cancer spend a pittance on prevention programs, such as public education.
occupyforanimals.net
Epidemiological and clinical studies have determined that most cancers are caused by smoking and by eating high-fat foods, foods high in animal protein, and foods containing artificial colors and other harmful additives. We can beat cancer by taking these human-derived, human-relevant data into account and implementing creative methods to encourage healthier lifestyle choices.
“Science has a responsibility to use animals to keep looking for cures for all the horrible diseases that people suffer from.”
Every year in the U.S., animal experimentation gobbles up billions of dollars (including 40 percent of all research funding from the National Institutes of Health), and nearly $3 trillion is spent on health care. While funding for animal experimentation and the number of animals used in experiments continues to increase, the U.S. still ranks 42nd in the world in life expectancy and has a high infant mortality rate compared to other developed countries. A 2014 review paper co-authored by a Yale School of Medicine professor in the prestigious medical journal The BMJ documented the overwhelming failure of experiments on animals to improve human health. It concluded that “if research conducted on animals continues to be unable to reasonably predict what can be expected in humans, the public’s continuing endorsement and funding of preclinical animal research seems misplaced.”
While incidences of heart disease and strokes have recently shown slight declines—because of a change in lifestyle factors, such as diet and smoking, rather than any medical advances—cancer rates continue to rise, and alcohol- and drug-treatment centers, prenatal care programs, community mental health clinics, and trauma units continue to close because they lack sufficient funds.
More human lives could be saved and more suffering prevented by educating people about the importance of avoiding fat and cholesterol, quitting smoking, reducing alcohol and other drug consumption, exercising regularly, and cleaning up the environment than by all the animal tests in the world.
“Many experiments are not painful to animals and are therefore justified.”
The only U.S. law that governs the use of animals in laboratories, the Animal Welfare Act (AWA), allows animals to be burned, shocked, poisoned, isolated, starved, forcibly restrained, addicted to drugs, and brain-damaged. No experiment, no matter how painful or trivial, is prohibited—and painkillers are not even required. Even when alternatives to the use of animals are available, U.S. law does not require that they be used—and often they aren’t. Because the AWA specifically excludes rats, mice, birds, and cold-blooded animals, more than 95 percent of the animals used in laboratories are not even covered by the minimal protection provided by federal laws. Because they aren’t protected, experimenters don’t even have to provide them with pain relief.
Between 2010 and 2014, nearly half a million animals—excluding mice, rats, birds, and cold-blooded animals—were subjected to painful experiments and not provided with pain relief. A 2009 survey by researchers at Newcastle University found that mice and rats who underwent painful, invasive procedures, such as skull surgeries, burn experiments, and spinal surgeries, were provided with post-procedural pain relief only about 20 percent of the time.
In addition to the actual pain of experiments, a comprehensive view of the situation for animals in laboratories should take into account the totality of the suffering imposed on them, including the stress of capture, transportation, and handling; the extreme confinement and unnatural living conditions; the deprivation that constitutes standard husbandry procedures; and the physical and psychological stress experienced by animals used for breeding, who endure repeated pregnancies, only to have their young torn away from them, sometimes immediately after birth.
Animals in laboratories endure lives of deprivation, isolation, stress, trauma, and depression even before they are enrolled in any sort of protocol. This fact is especially apparent when one considers the specialized needs of each species. In nature, many primates, including rhesus macaques and baboons, stay for many years or their entire lives with their families and troops. They spend hours together every day, grooming each other, foraging, playing, and making nests to sleep in each night. But in laboratories, primates are often caged alone. Laboratories often do not allow social interactions, provide family groups or companions, or offer grooming possibilities, nests, or surfaces softer than metal.
Indeed, in many laboratories, animals are handled roughly—even for routine monitoring procedures that fall outside the realm of an experimental protocol—and this only heightens their fear and stress. Video footage from inside laboratories shows that many animals cower in fear every time someone walks by their cage.
A 2004 article in Nature magazine indicated that mice housed in standard laboratory cages suffer from “impaired brain development, abnormal repetitive behaviors (stereotypies) and an anxious behavioral profile.” This appalling level of suffering results simply from standard housing conditions—before any sort of procedure is implemented.
A November 2004 article in Contemporary Topics in Laboratory Animal Science examined 80 published papers and concluded that “significant fear, stress, and possibly distress are predictable consequences of routine laboratory procedures” including seemingly benign practices such as blood collection and handling.
“We don’t want to use animals, but we don’t have any other options.”
The most significant trend in modern research is the recognition that animals rarely serve as good models for the human body. Human clinical and epidemiological studies, human tissue- and cell-based research methods, cadavers, sophisticated high-fidelity human-patient simulators, and computational models have the potential to be more reliable, more precise, less expensive, and more humane alternatives to experiments on animals. Advanced microchips that use real human cells and tissues to construct fully functioning postage stamp–size organs allow researchers to study diseases and also develop and test new drugs to treat them. Progressive scientists have used human brain cells to develop a model “microbrain,” which can be used to study tumors, as well as artificial skin and bone marrow. We can now test skin irritation using reconstructed human tissues (e.g., MatTek’s EpiDermTM), produce and test vaccines using human tissues, and perform pregnancy tests using blood samples instead of killing rabbits.
Brian Gunn/IAAPEA
Experimentation using animals persists not because it’s the best science but because of archaic habits, resistance to change, and a lack of outreach and education.
“Animals are here for humans to use. If we have to sacrifice 1,000 or 100,000 animals in the hope of benefiting one child, it’s worth it.”
If experimenting on one intellectually disabled person could benefit 1,000 children, would we do it? Of course not! Ethics dictate that the value of each life in and of itself cannot be superseded by its potential value to anyone else. Additionally, money wasted on experiments on animals is money that could instead be helping people, through the use of modern, human-relevant non-animal tests.
Experimenters claim a “right” to inflict pain on animals based on any number of arbitrary physical and cognitive characteristics, such as animals’ supposed lack of reason. But if lack of reason truly justified animal experimentation, experimenting on human beings with “inferior” mental capabilities, such as infants and the intellectually disabled, would also be acceptable.
The argument also ignores the reasoning ability of many animals, including pigs who demonstrate measurably sophisticated approaches to solving problems and primates who not only use tools but also teach their offspring how to use them.
The experimenters’ real argument is “might makes right.” They believe it’s acceptable to harm animals because they are weaker, because they look different, and because their pain is less important than human pain. This is not only cruel but also unethical.
What You Can Do
Tell Research-Funding Agencies to Kick Their Animal Experimentation Habit!
Virtually all federally funded research is paid for with your tax dollars. NIH needs to hear that you don’t want your tax dollars used to underwrite animal experiments, regardless of their purpose. When writing letters, be sure to make the following two points:
Animal experimentation is an inherently unethical practice, and you do not want your tax dollars used to support it.
Funding for biomedical research should be redirected into the use of epidemiological, clinical, in vitro, and computer-modeling studies instead of cruel and crude experiments on animals.
Please ensure that all correspondence is polite:
Francis S. Collins, M.D., Ph.D., Director
National Institutes of Health
Shannon Bldg., Rm. 126
1 Center Dr.
Bethesda, MD 20892
301-496-2433
francis.collins@nih.gov
Buy Cruelty Free!
There are many websites where you can find the names of cruelty free companies and products. Some are:
PETA’s searchable database
Leaping Bunny Program
Cruelty-Free Kitty Website
Beagle Freedom Project @ bfp.org
“We have moved away from studying human disease in humans. … We all drank the Kool-Aid on that one, me included. … The problem is that [animal testing] hasn’t worked, and it’s time we stopped dancing around the problem. … We need to refocus and adapt new methodologies for use in humans to understand disease biology in humans.” —Dr. Elias Zerhouni
Some Alternatives to the Use of Animals in Testing include:
- in vitro (test tube) test methods and models based on human cell and tissue cultures
- computerized patient-drug databases and virtual drug trials
- computer models and simulations
- stem cell and genetic testing methods
- non-invasive imaging techniques such as MRIs and CT Scans
- microdosing (in which humans are given very low quantities of a drug to test the effects on the body on the cellular level, without affecting the whole body system)
Please visit neavs.org or humanesociety.org for more detailed information on alternatives to animal testing or Google “alternatives to animal testing.” For general information on animal testing, please visit navs.org or Google “animal testing” and/or “vivisection.”
Excerpt from the book “Sacred Cows and Golden Geese – The Human Cost of Experiments on Animals” by C. Ray Greek, MD and Jean Swingle Greek, DVM